Treatments
The Pectus clinic is able to offer expert opinion on all forms of chest wall and pectus deformity. The treatment options discussed will depend on the type and severity of the pectus deformity. Other important considerations will be age, other associated musculoskeletal or cardiopulmonary problems and any other medical issues. In many cases, treatment may involve more than one option.

Psychological support
Both the feeling of the patient and attitudes of family members are very important in dealing with having a pectus deformity. Learning to live with the deformity and accepting it may well be an important strategy. Developing such coping strategies through psychological support and counselling may be helpful.
Physical therapy
Exercise and posture management is likely to help some of the associated problems with 'pectus posture' but alone there is less certain evidence of successfully treating the pectus deformity particularly more severe forms. For specific issues such as rib flaring and rounded shoulders there is some evidence that certain tailored exercise and stretching programs may improve the cosmetic appearance.

Bracing
The role of bracing for compliant pliable pectus carinatum has been used worldwide for several decades and is well established as standard treatment in many countries. However, in other countries including the UK expertise in bracing for pectus carinatum remains patchy, with little information or knowledge around its use.

Vacuum-bell device
The vacuum bell offers a non-surgical treatment of pectus excavatum. Initially met with some scepticism by doctors, recently several reports by surgeons experienced in treating pectus deformity as shown promising results. It can be used as both an alternative to surgical treatment of pectus excavatum.
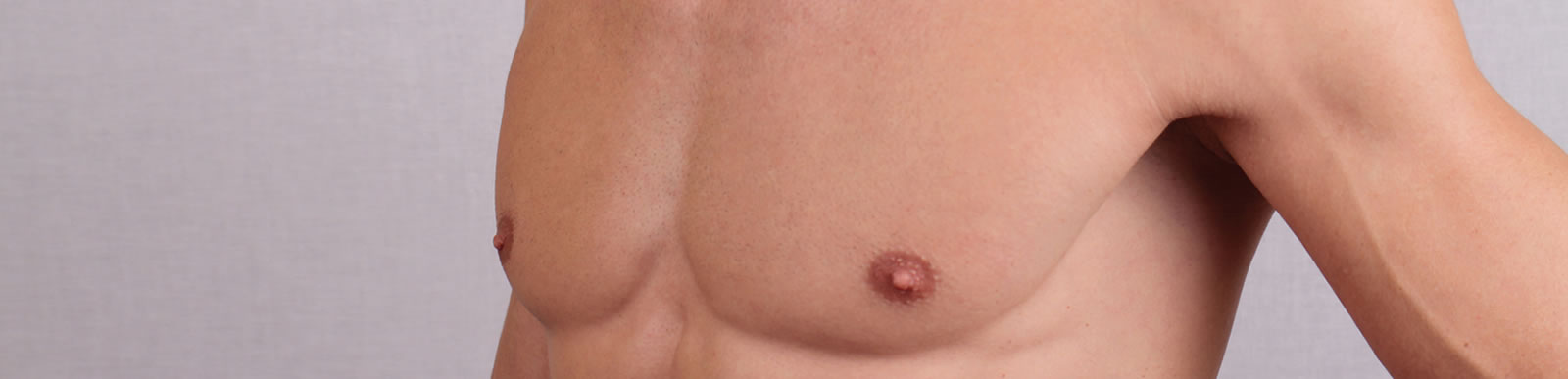
Pectus implants
Used typically to treat forms of pectus excavatum it involves placing a prosthetic implant under the skin in front of the breast bone to mask the deformity and therefore is a relatively minor surgical procedure.
Corrective Surgery
Surgery remains an important option in treating and correcting pectus deformities. Several types of operation are available and it's important that your surgeon is familiar with the different surgical options so that the type and severity of the pectus problem can be treated with the best approach safely and effectively.